Digitisation of Health

Chronic disease is costing governments and health providers trillions of dollars.
Despite good intentions, transparency and education are not enough.
Change needs to be led by embedding a deep understanding of the human condition into the digital experience.
With changing lifestyles and demographics, more than 75% of health care costs are due to chronic conditions such as heart disease, cancer, stroke, diabetes and arthritis. Mental health-related issues also cause significant ill health and disability. These conditions exacerbate in developing countries, as rising incomes, falling food prices and increasing urbanisation lead to global changes in diet, weight and physical inactivity.
There remains great potential for integrating prevention and care, and treating selected chronic diseases together, to improve health outcomes at scale, cost effectively.

Estimates indicate that the 4 most expensive disease groups are chronic and equate to 36% of all health expenditure. Australia spent an estimated $220.9 billion on health goods and services in 2020–21, taking the cost of chronic disease to $79bn, with just under half of all Australians having one or more chronic conditions. A similar picture paints in the US where half the country accounts for zero percent of all health care spending. The obesity epidemic has taken a horrible toll on Americans, and not just their health: It costs the country about $200 billion a year through health-related problems such as diabetes and heart disease. In all these cases, a lot can be be attributed to lifestyle.

Many chronic diseases share common risk factors that are preventable. Modifying these can reduce the risk of developing a chronic condition, leading to large health gains in the population through the reduction of illness and death. Chronic diseases are closely associated with modifiable risk factors such as smoking, physical inactivity, poor nutrition and the harmful use of alcohol. These behaviours contribute to the development of obesity, high blood pressure, and high cholesterol levels, which in turn lead to chronic disease. Seventy per cent of all cardiovascular disease mortality in Australia has been attributed to the combined effects of high blood pressure, high cholesterol and physical inactivity. Similar trends can be seen across the developed and developing world.
Transparency and education alone are not enough
Many agencies around the world have embarked on large initiatives to provide transparent access to health data and what they can do about it. The Australian government announced an initiative in 2020 aiming to:
- deliver safe, high-quality care in the right place at the right time
- prioritise prevention, and help people manage their health across their lifetime
- drive best-practice and performance using data and research
- improve efficiency and ensure financial sustainability.
America followed suit the following year with the 21st Century Cures, which mandated that healthcare providers give patients access to all the health information in their electronic medical records, without charge and without delay.
Certainly, digitisation is key for better, cheaper health. It can support continuity of care at national level and across borders, can assist in the reform of health systems and their transition to new care models, centred on people’s needs. Digitisation can enable a shift away from hospital-centred systems to more community-based and integrated care structures.
People who can access their own health information have been shown to have greater compliance with treatment protocols and a better understanding of their conditions
These initiatives have however been notoriously difficult to deliver and engage customers in. After 12 years and more than $2bn, hardly anyone is using the Australian My Health Record digital service. The latest annual report from the Australian Digital Health Agency shows just 2.69 million of the 23 million people registered for a My Health Record accessed it in 2020-21. Whilst consumers have high levels of willingness to share their health information with and between health care providers, research indicates more data flowing into the system, and improvements with respect to clinician and customer engagement are required.
Poor uptake can be avoided by building solutions using human centred design and making them fun. Being healthy and changing behaviour is hard. We don’t want to know if we are sick or dying or should be more disciplined. We fear shame and guilt. My Health Record is boring , with critical aspects for change completely absent. There is no empathy, personalization or indication of progress or success. By using game design and embedding game design elements and mechanics these mistakes can be avoided.
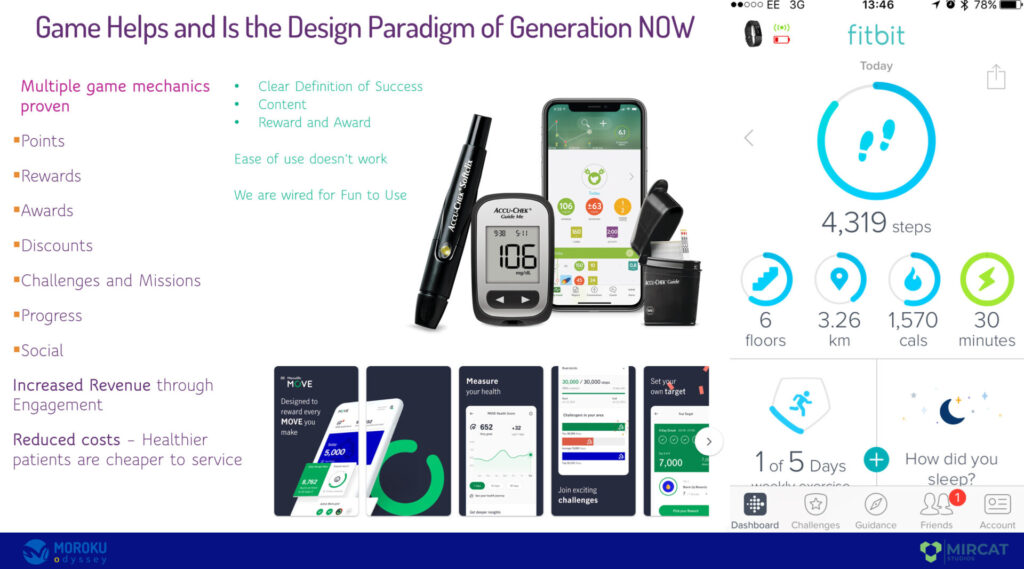
Indeed, whilst large initiatives struggle, eHealth apps are exploding in popularity. In recent years e-Health apps have become more popular and have now a projected market growth to US$102.3 Billion by 2023. They are getting the results and engaging Generation Now customers by employing game design and game mechanics into the essence of the digital experience. Unlike My Health Record, the applications that are working have a clear definition of success, that game designers call win states, content, reward and award.
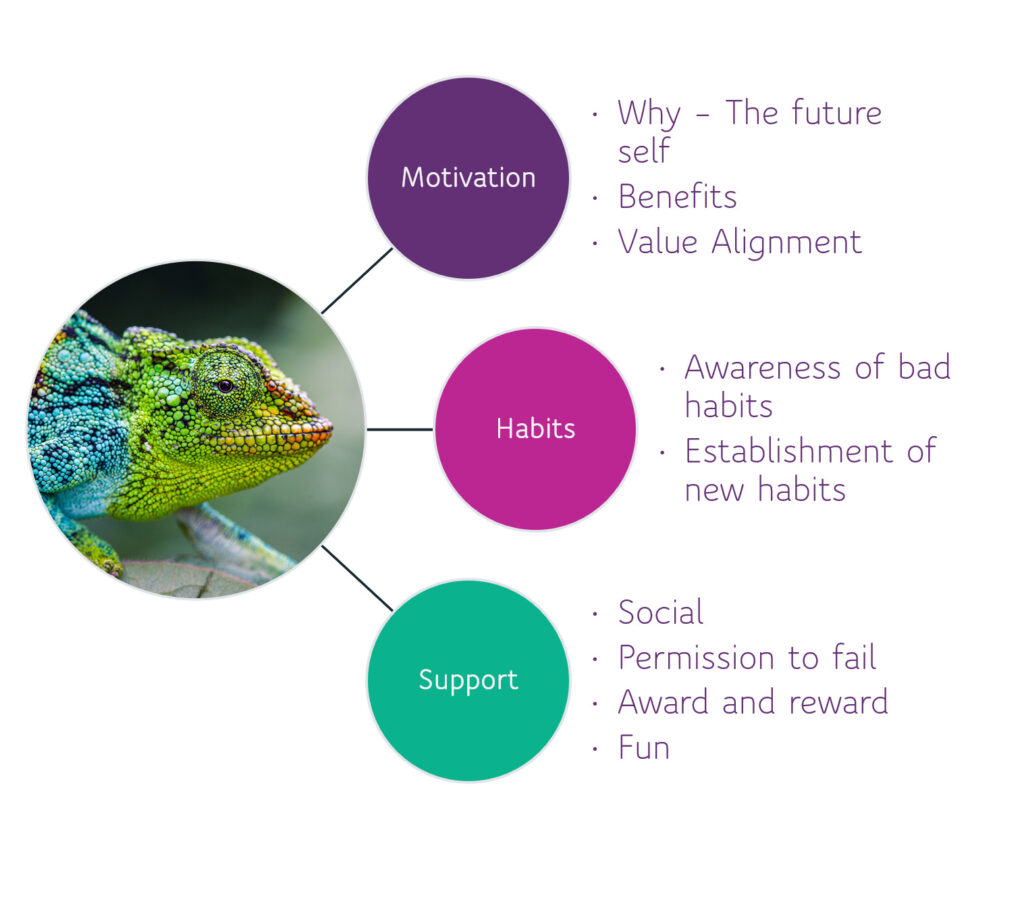
To the horror of clinicians and scientists who dedicate their lives to logic and reason, as a creed, we do thing snot because they are true, right, or logical, but because they deliver fitness payoffs and make us feel better. We are an emotional lot, constantly on the hunt for validation and short-term fixes to feeling, better or at least OK. For digital applications to drive change, they must incorporate three key elements: Motivation to use, Habits to be formed, Support for success and failure, through the use of fun and social.
In recognition of the important of an overarching wellness approach, Australia has launched a well being framework. Set up to measure what matters, the framework is made up of about 50 indicators the government will track through time to track the extent to which Australia is :
healthy
secure
sustainable
cohesive
prosperous.
Moroku is a digital service provider focused on delivering solutions that help customers take on challenges and build wellness through improved habits. It does this using its expertise in serious game design and delivery. The use of game as an architecture is the most powerful method available to us to engage people and take them on a journey of mastery. The approach harnesses human psychology and behavioural economics to build empathy and create user journeys that exploit our innate desire to compete, win and have fun as we take on challenges, building skills and better habits.
Whilst other providers are stuck in making systems easy to use, Moroku recognises that being healthy is not easy and therefore a linear, hierarchical design paradigm around ease of use doesn’t work. What is required is a design paradigm that recognises there is failure, going forwards as well as backwards and the necessity to persevere with the struggle through reward and engagement, based on the way all animals learn key life skills, game.
Our vision is for a platform that brings patient health records and information into a central location for authorized practitioners to access in the development of outcomes to speed and improve delivery of those outcomes as well as for individual citizens to go on their own health journeys, build plans, habits, and lifestyles commensurate with living well.
Service providers want to deepen customer relationships. This requires a platform with Emotional Intelligence. Hyper personalisation based on AI player maps that know where customers are, where they have come from and where they are going, is Moroku’s unique and powerful model of doing this. Moroku Odyssey is an orchestration and engagement platform for services providers. Operating from the cloud it integrates securely into the digital infrastructure to drive engagement and promote loyalty, by building empathy and support for life’s hard work.